This is an excerpt from my rock bottom of 2017: "I no longer recognise myself - physically or (worse) as the person I used to be: happy, confident, always glass-half-full." And this is how a stranger put me back together. I was four months into the worst eczema flare up I'd ever known when I met Justine Hextall, a dermatologist with over ten years' experience. By this point, I'd almost gotten used to having people's eyes on my skin - strangers staring at me on the tube, well-meaning colleagues asking if I'd been burned - as I sunk further within myself. Almost.
What had started as small and angry, peculiarly-defined patches of red on my wrists had spread to my arms and across my back, up my neck and, finally, over my face. GPs hadn't been able to help me - in fact, in several appointments, I'd watched them Google which steroids to give me next - and a walk-in centre sent me away without even looking at my skin, having prescribed me antibiotics and drowsy pills that I didn't want to take.
Victoria consulted dermatologist Justine Hextall after suffering a severe eczema flare up
RELATED: 7 dermatologist tips for managing eczema
Looking back at the weeks that followed, I wish I hadn't spent so much time misdiagnosing myself and coming up with new action plans based on my own medical knowledge (which is zero, FYI). I just desperately wanted to believe the wellness industry and its promise that these things are all treatable with smoothies and self-care. In reality, I'd never been less relaxed or more restricted with what I could eat/wear/do. It was also quickly draining my bank account - turns out that buying 100% silk or cotton of everything is expensive...
Formerly confident, I no longer wanted to stand close enough to people to have a conversation for fear that they'd be disgusted by my flaking face. My mood was getting lower and I had few remaining vices; sweating off my frustration in the gym made the redness flare, and even aimless scrolling on social media bombarded me with images of perfect skin. I felt equal parts a victim of my own body and guilty for even complaining; I knew far, far worse things are faced by people every day, but this was my every day and it showed no sign of relenting. I was desperate.
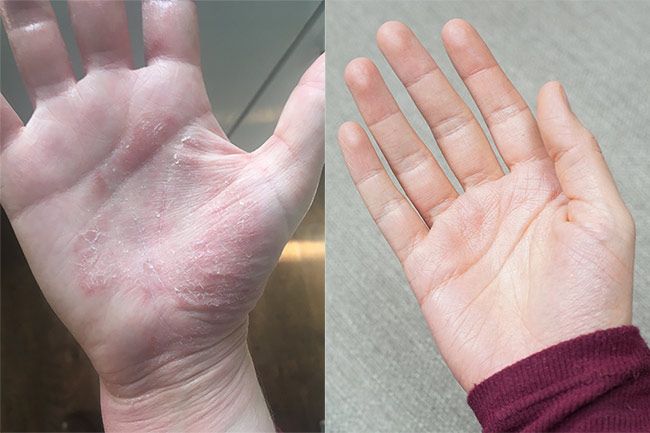
The eczema on Victoria's hands before and after treatment
So when Justine diagnosed me within 30-seconds of meeting me, I blubbed. This wasn't about stress, or diet, or the changing of the seasons - it was a very specific type of skin infection triggering a flare which, she assured me, with a bit of time, was all entirely treatable. Eczema progress ebbs and flows as the skin heals and adapts, so I didn't want to get my hopes up, but she doesn't make promises she can't keep. After a month, not only had the infection and the eczema gone away, but I'd gotten my glow back from two game-changing skincare brands on her recommendation.
Now, for the first time ever, people are grilling me for my skincare secrets: I start every day by treating my face to a cleanse and tone with the La Roche Posay Toleriane trio, and nourishing my skin with Avene shower oil and body cream. Never really the pampering type, I've been converted by the five-minute magic of the Avene face mask, and I won't go to sleep without first applying the La Roche Posay night cream.
MORE: Treating baby eczema - tips from the experts
From this most literal of battles in finding comfort in your own skin, I learned the importance of seeing someone who knows what they're talking about - forgoing Google and miracle recovery stories for an expert opinion - and, even better, someone who understands you. Justine could tell this was a physical ailment and so much more. By taking away the guesswork and the guilt, she left me with one job: to follow simple instructions. And so, just five weeks after our first meeting - having been on-hand throughout - I sent Justine a makeup-free selfie of a me that I actually recognised: happy.
Justine's treatment has transformed Victoria's skin
Justine says: "When I first consulted with you, firstly I was struck by the longevity of your skin eruption despite using topical steroids for weeks. Secondly your distress was palpable and the impact on your day to day life was significant - I really wanted to help you! You were able to show me several pictures of your evolving skin rash and I noticed how well demarcated the annular skin lesions were. Your facial rash looked very inflamed but again there was a definite edge and sharp cut off. Although you had the classic distribution of eczema and a long history of this skin diagnosis, I didn't want to assume anything."
She added: "Two facts were striking: When you were in a hot climate the rash became much more pronounced. Secondly, on direct questioning you admitted that when the steroid was applied the centre cleared but the outside edge, if anything became for pronounced. I knew that applying steroid cream to a fungal or yeast infection could produce this reaction.
Watch for Justine Hextall's advice on the causes and treatment for eczema
RELATED: See the latest skincare features here
"I decided to treat you with anti-fungal cream at first to see the response and then add in a combination of anti-fungal cream and steroid to reduce the inflammation as there was clearly also an underlying eczema that had flared. I had to walk a careful line between treating infection and also reducing the skin inflammation.
"Immediately the skin became less red and, as the inflammation and swelling settled the skin became dry and peeling as you might see after a sunburn. To this end I made sure I recommended the gentlest cleanser and hydrating moisturiser to start to repair the skin barrier. I recommended the Toleriane range by La Roche Posay as it is specifically formulated for sensitive skin. Watching your skin improve and with that seeing how buoyed you were was fantastic. I feel you now a have an excellent skin regime that is keeping your skin calm and hydrated - and crucially protecting your skin barrier- hence your fantastic healthy glow!"
What causes eczema?
Whilst it is common for eczema to appear on babies, it can develop at any point in a person's life. with eczema prone skin there is often structural changes to the skin barrier , as such individuals are less likely to have and maintain properly hydrated skin and may also be more prone to contact irritants and infection.
Whilst for many it may be a long-term skin condition to manage, for others it may arise as a one-off reaction to particular chemicals or fragrances.
Different types of eczema
There are different types of eczema , for example atopic eczema that is common in childhood and often associated with hay fever and asthma. Irritant eczema can arise for example in those that are frequently washing hands e.g. hairdressers , new mothers etc. If an allergic product is put onto skin this can cause what is referred to as contact eczema. Common allergens include perfumes, nickel, hair dye and preservatives.
Steroid creams - how long can you use them for?
Steroid creams are a common treatment for eczema, with different strengths prescribed depending on the thickness of the skin in the area you are treating (the fine areas on your face, for example, will be prescribed a lower percentage of steroid). They are typically prescribed to be used over a few days / weeks rather than for prolonged period. It is common to start with a stronger steroid for a short period to rapidly reduce the inflammation followed by a weaker steroid to reduce the risk of a rebound flair.
Justine's recommendation is to ensure that you complete the time period prescribed to you, applying the creams even if the symptoms disappear during this time - this is known as treating beyond the point of "clinical clearance". By treating it in this way there is less risk of a rebound flair. Prolonged use of steroids can result in thinning of the skin and in some cases stretch marks can develop. If you are prescribed additional steroid cream use by your doctor or dermatologist, it is usually recommended that your skin is afforded a break between treatments. If you are unsure, check with your doctor and do not use for prolonged periods without expert advice.
Diet changes: foods to avoid if you have eczema
Justine's advice is to pursue a healthy, balanced diet - filled with fresh fruits and vegetables and foods that are rich in antioxidants to keep your skin healthy. If you suspect that certain ingredients (such as caffeine, alcohol, dairy, or acidic foods like tomatoes) are irritating your skin, start by keeping a food diary over a two-week period and noting any reactions. You can then eliminate those foods for a short period to see if there is an improvement.
Lifestyle changes: what you can do to ease eczema symptoms
Create barriers to irritants - like wearing rubber gloves to avoid direct contact with washing up liquid or cleaning products. If you have eczema on your eyelids, applying a layer of moisturiser before showering or washing your hair can help stop irritating products from making direct contact with inflamed skin. Cotton sheets and clothing is often more comfortable on the skin and allows it to breathe, whereas other manmade fibres can trap in heat and moisture (the perfect conditions in for an irritation or infection to develop).