Skin cancer is the most common form of cancer in the UK, but most skin cancers can be cured if detected early, according to the British Skin Foundation.
HELLO! caught up with Dr. Peter Dziewulski to better understand the disease, from spotting the signs early to treatment options available. He detailed the different types of skin cancer and shared ways to avoid catching it in the first place.
Read on for his detailed explainer on skin cancer.
What is skin cancer?
Skin cancer refers to a group of cancers arising from the skin. Skin cancer is one of the most common cancers in the world. The groups can be divided into melanoma and non-melanoma skin cancer.
Non-melanoma skin cancers refer to a group of cancers that arise in the upper layers of the skin and grow slowly. In the UK, around 147,000 new cases of non-melanoma skin cancer are diagnosed each year. It affects more men than women and is more common in the elderly.
Melanoma is a less common type of skin cancer but can behave in a more aggressive way and can be more serious. Around 16,700 people are diagnosed with melanoma in the UK each year. The number of people diagnosed with melanoma has increased over the last few decades.
What are the different types of skin cancer?
Non melanoma skin cancer (NMSC)
This includes 2 main types: basal cell carcinoma (BCC), also known as a rodent ulcer, starts in the cells lining the bottom of the epidermis and accounts for about 75 in every 100 skin cancers.
The other type is squamous cell carcinoma (SCC), which starts in the cells lining the top of the epidermis and accounts for about 20 in every 100 skin cancers.
The two types are named after the skin cells where the cancer develops. It's possible for a non-melanoma skin cancer to be a mixture of both these types. There are other types of NMSC that are much less common and include Merkel Cell Carcinoma, Adnexal (mainly sweat gland) tumours and Cutaneous Lymphomas (from white blood cells). Non melanoma skin cancer is different from melanoma.
What is melanoma skin cancer?
Melanoma skin cancer is the fifth most common cancer overall in the UK. The number of people diagnosed with melanoma has increased over the last few decades.
Melanoma is the type of skin cancer that arises from pigment cells lying deeper in the skin. It often develops from a pre-existing mole. This can be a mole that is already on the skin or a new mole or lesion that has recently appeared.
Melanoma starts in cells in the skin called melanocytes. These cells are in the deep layer of the epidermis between the layer of basal cells.
What causes melanoma?
The risk of developing melanoma depends on many things including lifestyle factors and some medical conditions. In the UK, around 85 out of 100 melanomas (around 85%) are caused by too much ultraviolet radiation (sun damage). Ultraviolet light comes from the sun or sunbeds.
Sunburn increases the risk of melanoma. Research shows that the type of ultraviolet light used in sunbeds (UVA) can cause all types of skin cancer.
The risk of melanoma increases with age. In the UK, more than 25 out of 100 people (more than 25%) diagnosed with melanoma are aged 75 and over, though younger people can also develop it.
It's rare for black people in the UK to get melanoma. If African or Asian people do get melanoma, it is usually a type of melanoma that develops on the soles of the feet or the palms of the hands (acral lentiginous melanoma) or underneath the nail.
READ: How my breast cancer diagnosis took me on the path to unexpected happiness
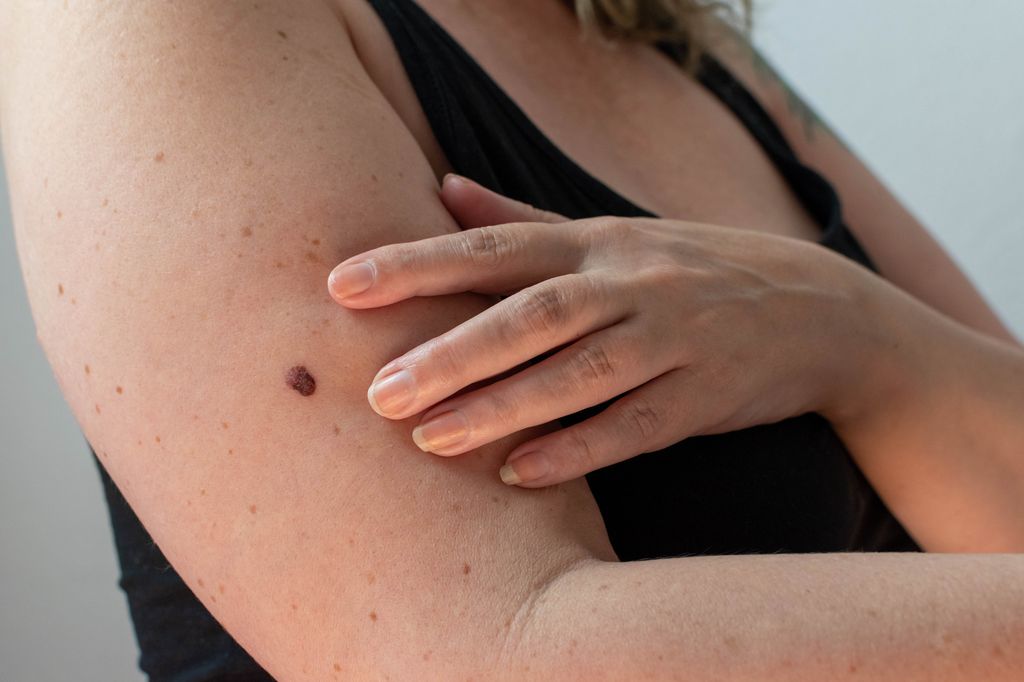
How can you spot the early signs of skin cancer?
Skin cancers can have a variety of appearances and the symptoms can vary. Common symptoms of skin cancer include an ulcer or sore, or area of skin that:
- Doesn't heal within four weeks
- Looks unusual and/or is painful
- Is itchy, bleeds, crusts, or scabs for more than four weeks. The sore can look see through, shiny and pink or pearly white. It can also look red. It may feel sore, rough and have raised edges.
Look at hard to see parts of your body
We might miss cancer if it's somewhere hard to see, such as our back.
To look at areas that can’t be seen easily, mirrors may be useful, mobile phone camera photos or asking a partner or a friend to look can all be helpful. Taking photos of anything that doesn't look quite right can be helpful particularly if the lump or mole is changing. You can show these pictures to your doctor if you're concerned.
How to spot skin cancer
Regularly self-checking the skin for signs of skin cancer can help lead to an early diagnosis and increase the chance of successful treatment.
Using the ABCDE system is helpful:
A – Asymmetrical - Melanomas often have an uneven shape. The two halves of the area may be different shapes (asymmetrical).
B – Border - Melanomas are more likely to have irregular edges (border) and can be blurred or jagged.
C – Colour - Melanomas often have an uneven colour and contain more than one shade of black, brown and pink.
D – Diameter - Most melanomas are more than 6mm wide.
E – Evolving – or changing in size, shape or colour. In addition, bleeding, itching, or becoming crusty.
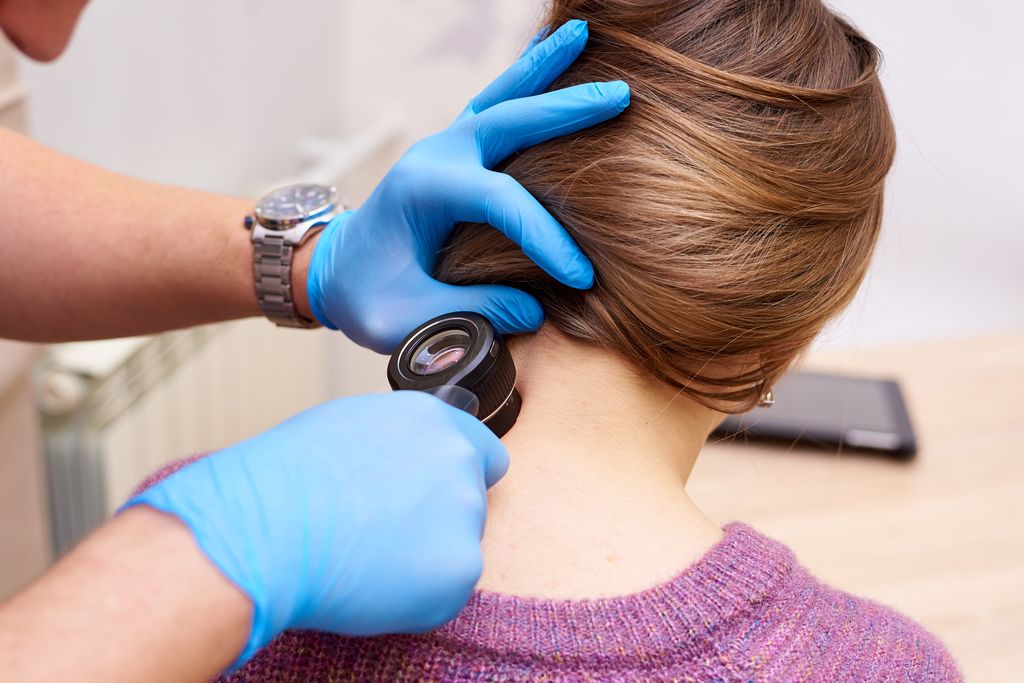
When to see a doctor about skin cancer
If there are concerns about any changes then a visit to your doctor should be made. They may wish to examine the skin with a dermatoscope and/or refer on to a specialist (usually a dermatologist).
The specialist will examine the skin and arrange removal of the mole or abnormal area of skin to see if it might be a skin cancer. This is called an excision biopsy. The abnormal area or mole is sent to a laboratory. A specialist doctor (pathologist) looks at the tissue under a microscope to give a definitive diagnosis.
Skin cancer treatment
This may be all the treatment that is required. Often a second operation needs to be undertaken to ensure complete removal of the cancer and to reduce the risk of the cancer coming back in the same area. This is called a wide local excision. This is usually done under a local anaesthetic (like the dentist) as an outpatient or same day case.
Surgery for skin cancer
Surgery is the main treatment for non-melanoma skin cancer. It involves removing the cancerous tumour and some of the surrounding skin. Other treatments for non-melanoma skin cancer include freezing (cryotherapy), anti-cancer creams, radiotherapy and a form of light treatment called photodynamic therapy (PDT).
At least 9 out of 10 non-melanoma skin cancer cases are successfully cured.
If a larger piece of skin is removed as happens for melanomas or in areas where there is not much loose skin, then the surgeon may need to replace the missing skin with either a skin graft or a flap. These are pieces of skin that are taken with (flap) or without (graft) their own blood supply to replace the missing skin. This procedure is usually undertaken by a plastic surgeon.
For patients with certain types of higher risk melanoma a lymph node biopsy (Sentinel Lymph Node Biopsy) is offered to see if melanoma cells have travelled to the local lymph nodes. This test identifies patients who might benefit from further treatment (either surgery or drug therapy). This procedure is usually undertaken under a general anaesthetic.
In certain patients with higher risk melanomas or those patients with a positive sentinel lymph node test imaging is used (CT, MRI, PET CT scans) to see if the melanoma has spread to other organs.
For patients with melanoma that has spread to the lymph glands or further afield (liver, lungs, brain) then patients will be referred on to an Oncologist who use drugs to treat the disease. The commonly used types are:
Immunotherapy drugs that help the body’s natural defence system or immune system to attack the cancer.
Targeted cancer drugs that work by targeting the differences in cancer cells that help them to grow and survive.
Researchers continue to look at new and different treatments with targeted cancer drugs and immunotherapies to identify more successful ways of treating the disease.
READ: How my cancer diagnosis transformed my relationship with exercise'
Skin cancer survival
Survival depends on many factors. Survival statistics are obtained by studying large numbers of patients to see what happens to them. These statistics are a guide but can’t accurately predict what will happen to any individual patient.
In general people with melanoma in England almost all people (almost 100%) will survive their melanoma for one year or more after they are diagnosed, around 90 out of every 100 people (around 90%) will survive their melanoma for five years or more after diagnosis, more than 85 out of every 100 people (more than 85%) will survive their melanoma for 10 years or more after they are diagnosed.